Penanganan obstetri prolaps uterus pascapersalinan pada sapi Angus potong skala kecil
Prolaps uterus pascapersalinan merupakan keadaan darurat reproduksi yang serius pada sapi yang dapat mengakibatkan perdarahan, kontaminasi, syok, dan kematian jika tidak segera ditangani. Laporan kasus ini menggambarkan keberhasilan penanganan prolaps uterus pada sapi Angus berumur 5 tahun yang dipelihara dalam sistem pertanian skala kecil tradisional. Hewan tersebut ditemukan dalam posisi berbaring miring satu hari setelah melahirkan, dengan prolaps uterus lengkap dan kemampuan berdiri yang terganggu. Pemeriksaan klinis menunjukkan suhu rektal 38,5 °C. Penanganan segera melibatkan reposisi manual uterus yang prolaps dengan bantuan epidural, diikuti dengan penjahitan retensi vulva menggunakan pola jahitan terputus sederhana. Terapi tambahan meliputi amoksisilin, vitamin B12, dan antihistamin. Pemulihan klinis tercapai tanpa kekambuhan atau komplikasi pasca perawatan.
■ INTRODUCTION
Uterine prolapse is a life-threatening postpartum emergency in cattle, occurring within hours after calving (Rees, 2016)). The condition involves complete uterine eversion through the vulva, caused by uterine atony and abdominal straining. Predisposing factors include dystocia, hypocalcemia, prolonged parturition, and excessive traction during fetal extraction (Carluccio et al., 2020). Without prompt management, uterine prolapse can lead to hemorrhage, contamination, metritis, hypovolemic shock, and death. Understanding its pathophysiology and ensuring timely clinical management are crucial for animal welfare, reproductive performance, and farm economics.
This case demonstrates successful clinical outcomes under traditional smallholder farming conditions with limited veterinary access. It shows how rapid recognition and intervention through manual repositioning, vulvar retention suturing, and supportive therapy can yield favorable outcomes in obstetrical emergencies. This case highlights the critical role of farmers' awareness in identifying early signs and seeking prompt assistance, as delays may determine recovery versus mortality.
Previous evidence reported a 35% prevalence of uterine prolapse in beef cows at the Besuki Animal Health Center, Situbondo, with housing, age, parity, and dystocia as significant risk factors (Mardotillah et al., 2024)). This study examined the clinical management of uterine prolapse in beef cattle and its relevance to veterinary medicine and farmer education, focusing on emergency obstetric handling, nutritional and calcium balance, and post-treatment care for reproductive health and herd productivity.
■ CASE
Signalment: Angus beef cow, 5 years old, body condition score (BCS) 3, second calving, maintained in an individual cage under traditional farming conditions.
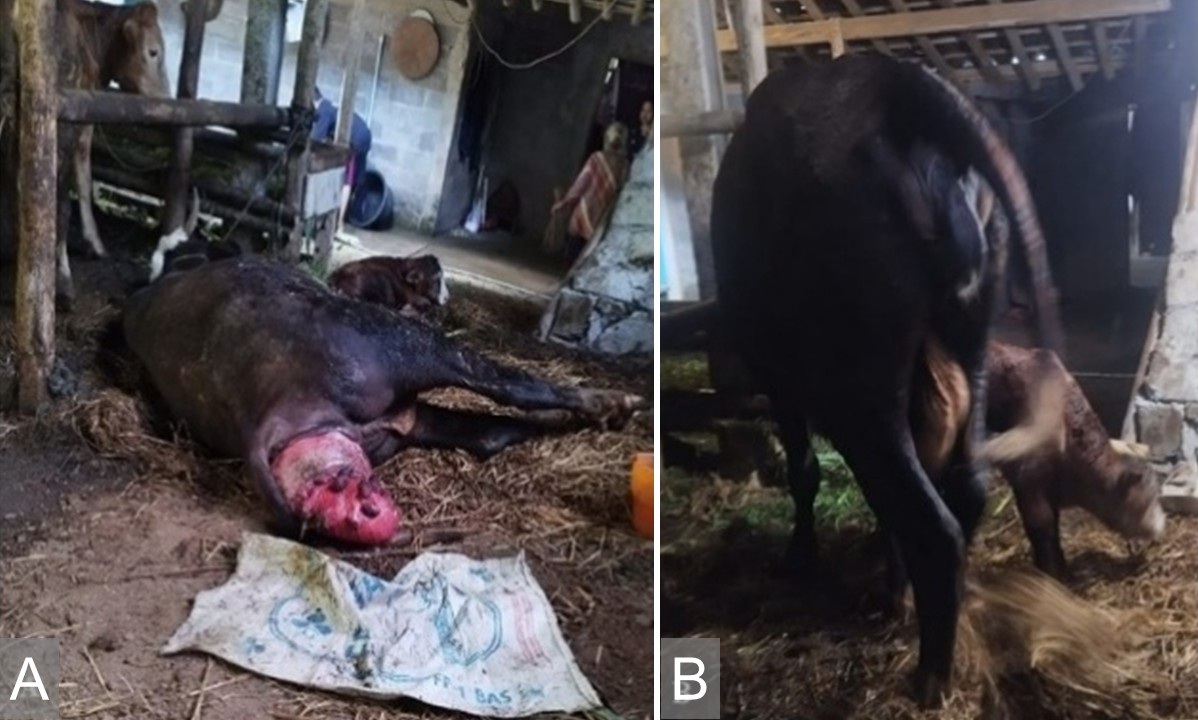
Anamnesis: One day postpartum, the cow was found collapsed in lateral recumbency with the uterus completely prolapsed and exposed to contamination (Figure 1).
Clinical signs: The animal showed lateral recumbency. A partial uterine prolapse extending 15 cm beyond the vulva was observed. Vital signs included a temperature of 38.5°C, heart rate of 80 bpm, and respiratory rate of 32 breaths/min. No severe hemorrhage was observed.
Differential diagnoses: Vaginal prolapse, retained fetal membranes, partial uterine eversion, and severe postpartum vaginal edema.
Diagnoses: Postpartum uterine prolapse.
Prognosis: Fausta.
Therapy: The prolapsed uterus was cleansed with sterile saline and treated with hypertonic saline (NaCl 7.2%, Vetitex) to reduce edema. Epidural anesthesia (lidocaine 50-100 mg/100-300 kg BW [Lidocaine HCl 2%, Pharos]) was administered to prevent straining. Manual repositioning began with the cervix and was followed by Bühner retention sutures on the vulva. Treatment included 15 mg/kg BW amoxicillin (Amoxi 15 LA, Avindo), vitamin B12 komplek 0.5 mL/10 kg BW (Injekvit B-Plex, Medion), and antihistamine 25-50 mg/100-300 kg BW diphenhydramine HCl (Vetadryl Inj, Sanbe) to prevent infection, aid recovery, and reduce inflammation.
Figure 1.Postpartum uterine prolapse and clinical outcomes following treatment in an Angus beef cow. (A) Prolapsed uterus after parturition, showing uterine eversion with exposed mucosal tissue. (B) Post-treatment condition following manual repositioning and supportive management, indicating successful uterine replacement.
■ RESULTS AND DISCUSSION
In the present case, uterine prolapse was most likely precipitated by uterine atony occurring shortly after parturition when inadequate myometrial contraction failed to maintain the uterus in its normal anatomical position. Several contributing factors may have further compromised uterine tone, including calcium deficiency, physical exhaustion following prolonged labor, and excessive traction during delivery, all of which are recognized as predisposing conditions for uterine prolapse in cattle (Dubuc et al., 2010). Early detection and immediate treatment are pivotal in preventing progression to more severe complications, such as hemorrhage, contamination, tissue trauma, and necrosis of the exposed uterus (Miesner & Anderson, 2008).
The favorable prognosis (fausta) observed in this case was primarily attributed to prompt and appropriate clinical intervention. Epidural anesthesia played a critical role in suppressing abdominal straining, thereby facilitating safer and more controlled uterine repositioning (Dorn 2023). Careful manual replacement of the prolapsed uterus, followed by the application of retention sutures, was essential to minimize the risk of recurrence and stabilize the reproductive tract. In addition, supportive therapy contributed to systemic recovery during the postpartum period, and close monitoring over the subsequent 7 days confirmed that the uterus remained in the correct position and that no secondary infection developed. Collectively, this management approach highlights the effectiveness of timely obstetrical intervention in restoring reproductive integrity and preventing long-term reproductive sequelae. Importantly, the successful outcome achieved under smallholder farming conditions underscores the practical challenges of managing uterine prolapse in resource-limited settings, where access to veterinary services, facilities, and optimal environmental hygiene may be restricted.
The therapeutic administration of amoxicillin provided broad-spectrum antibacterial coverage, thereby reducing the risk of metritis and septicemia. Vitamin B12 was administered to support hematologic and metabolic recovery during the postpartum period, whereas Vetadryl functioned as an antihistaminic agent to help alleviate inflammatory responses and discomfort. To reduce the likelihood of such cases, farmers should ensure an adequate mineral balance-particularly calcium-during the prepartum and postpartum periods, provide nutritionally balanced feed, and closely supervise animals during calving (Kang et al., 2025). Ultimately, sound obstetrical management and early clinical intervention remain the most effective strategies for preventing uterine prolapse and preserving reproductive performance in beef cattle.
■ CONCLUSION
Early recognition and prompt management of uterine prolapse in beef cattle can enable complete recovery. Success requires timely uterine repositioning, retention suturing, and supportive therapy to prevent complications. In smallholder systems, prevention should focus on proper nutrition, calcium balance, and periparturient monitoring to reduce the incidence of prolapse.
Referensi
- Carluccio A., Amicis D., Probo I., Giangaspero M., Veronesi B., C M.. Prevalence, survival and subsequent fertility of dairy and beef cows with uterine prolapse. Acta Veterinaria Hungarica. 2020; 68(1)DOI
- Dubuc J., Duffield T.F., Leslie K.E., Walton J.S., Leblanc S.J.. Risk factors for postpartum uterine diseases in dairy cows. Journal of Dairy Science. 2010; 93(12)DOI
- Kang D., Lungu S.E., Danso F., Dzou C.F., Chen Y., Zheng X., Zhou G.. Animal health and nutrition: Metabolic disorders in cattle and improvement strategies. Frontiers in Veterinary Science. 2025; 12DOI
- Mardotillah K., Utama S., Safitri E., Hermadi H.A., Madyawati S.P., Legowo D., Hasib A.. Uterine prolapse and related factors in beef cow at the Besuki Animal Health Center, Situbondo regency, East Java, Indonesia. Ovozoa Journal of Animal Reproduction. 2024; 13(3)DOI
- Miesner M.D., Anderson D.E.. Veterinary Clinics of North America: Food Animal Practice. 2008. DOI
- Rees G.. Practice. 2016. DOI
Carluccio A, De Amicis I, Probo M, Giangaspero B, Veronesi MC. 2020. Prevalence, survival and subsequent fertility of dairy and beef cows with uterine prolapse. Acta Veterinaria Hungarica. 68(1):91-94. https://doi.org/10.1556/004.2020.00017 | PMid:32384072
Dubuc J, Duffield TF, Leslie KE, Walton JS, LeBlanc SJ. 2010. Risk factors for postpartum uterine diseases in dairy cows. Journal of Dairy Science. 93(12):5764-5771. https://doi.org/10.3168/jds.2010-3429 | PMid:21094748
Kang D, Lungu SE, Danso F, Dzou CF, Chen Y, Zheng X, Zhou G. 2025. Animal health and nutrition: Metabolic disorders in cattle and improvement strategies. Frontiers in Veterinary Science. 12:1470391. https://doi.org/10.3389/fvets.2025.1470391 | PMid:40201075 PMCid:PMC11977490
Mardotillah K, Utama S, Safitri E, Hermadi HA, Madyawati SP, Legowo D, Hasib A. 2024. Uterine prolapse and related factors in beef cow at the Besuki Animal Health Center, Situbondo regency, East Java, Indonesia. Ovozoa Journal of Animal Reproduction. 13(3):146-152. https://doi.org/10.20473/ovz.v13i3.2024.146-152
Miesner MD, Anderson DE. 2008. Management of uterine and vaginal prolapse in the bovine. Veterinary Clinics of North America: Food Animal Practice. 24(2):409-419. https://doi.org/10.1016/j.cvfa.2008.02.008 | PMid:18471579
Rees G. 2016. Postpartum emergencies in cows. In Practice. 38(1):23-31. https://doi.org/10.1136/inp.h6407
Hak Cipta (c) 2026 CC-BY-SA

Artikel ini berlisensiCreative Commons Attribution-ShareAlike 4.0 International License.
Karya ini dilisensikan di bawah Creative Commons Attribution-ShareAlike 4.0 International License (CC BY-SA 4.0).
Lisensi ini mengizinkan siapa pun untuk menyalin, membagikan, menggunakan kembali, mengadaptasi, mengubah, dan mengembangkan karya ini dalam media atau format apa pun, termasuk untuk tujuan komersial, dengan syarat mencantumkan atribusi yang sesuai kepada penulis/pencipta asli, menyertakan tautan ke lisensi, dan menjelaskan jika ada perubahan yang dilakukan.
Apabila karya ini diadaptasi atau dimodifikasi, hasil adaptasinya harus didistribusikan dengan lisensi yang sama atau lisensi yang kompatibel.

















